Introduction
Effective communication between physician and patient is critical in healthcare delivery to ensure correct diagnosis, subsequent course of treatment, and billing/reimbursement. Both parties must be able to understand what the other is saying and later remember the details on the exchange.
Recent research has shown how incomplete medical records “pose a serious challenge to the health care of patients” and that “the biggest reasons for missing health information are communication and education.”
The completeness of information captured during physician/patient encounters varies broadly – whether it is an in-person visit that takes place in a brick-and-mortar building or a telehealth appointment facilitated by technology.
The University of Central Florida (UCF) and CirrusMD partnered on a National Science Foundation (NSF) funded research project to characterize the data completeness of chat-based episodes of care on the CirrusMD Physician-first Care & Guidance virtual care platform. They also identified a correlation between high data completeness and positive patient experience and outcomes.
This paper presents the outcomes of this research and opportunities to apply artificial intelligence (AI) and machine learning (ML) algorithms to 100% accurate chat-based data sets for greater physician empowerment and episode of care efficiency.

Communication breakdowns in care encounters
“A positive patient experience is the result of multiple factors before, during, and after the patient encounter, but chief among them is effective doctor-patient communication,” stated the authors of an article published in the American Academy of Family Physicians (AAFP FPJ) Journal.
In the current healthcare environment, where physicians face productivity pressures, they have less time to spend with each patient, “which can impede effective patient–physician communication.”
Often physician-patient encounters are not well documented, especially for the patient. In addition, conventional care models prohibit both physician and patient from asking questions after the episode of care has concluded. For example, the patient forgot to mention sleeplessness during a physician visit where the primary concern was a sprained ankle. Or the physician later remembers some aspect of the conversation that could indicate the patient was suffering from anxiety and regrets not asking them about it. Both can follow up after the fact but that might require an additional visit, which means additional time and costs.

Virtual care gaps
Communication gaps occur not only during in-person patient/physician visits, but also during virtual care encounters. When an episode of care happens via a video platform or over the telephone, there is still the risk that one of the parties fails to document or remember part of the visit after it has concluded.
In situations where the patient or physician needs clarity or additional information, it can be challenging — and costly — to reconnect. It will likely require a subsequent visit. Multiple episodes of follow up care lead to increased costs and greater time commitment from physicians who often don’t have time to spare.
There is technology available to transcribe video and telephone conversations between physician and patient, but it occurs after the fact and is not 100% accurate. Furthermore the transcription is generally available to the physician post-encounter for documentation and billing purposes, but not to the patient. If one or both of the parties has questions or is lacking information, they cannot connect in the moment because the episode of care has ended. This again leads to time consuming, inconvenient, and costly follow up care.

Clinical and financial consequences
The consequences of poor communication and information capture during patient/physician encounters are well documented. As reported in the American Family Physician journal, “Poor communication can lead to a medical error when a patient does not report their allergies or health history to a physician, or when a physician does not correctly or thoroughly record a medical history or medication list.”
The authors of an AAFP FPJ journal article offered this insight
and advice to family physicians:
“Patients often come away from their visits not knowing the actual name of their diagnosis, the reasons for their new medications, possible side effects, or what to expect next. It is important to explain things clearly — your thoughts, diagnoses, treatment recommendations, and plan for follow up — and to write down all new diagnoses and medications to allow full patient engagement…. Even if you have explained things thoroughly during the visit, patients are often overwhelmed with information and may not hear everything correctly.”
Additionally, poor communication and documentation during care episodes can lead to financial losses when a physician pressured to work efficiently fails to correctly capture and code billable services. Another challenge is
communicating information needed for referrals, with the American College of Physicians (ACP) reporting that up to 50% of referrals are not completed.
UCF NSF-funded research on AI in telehealth
University of Central Florida (UCF), a research leader in engineering, computer science and healthcare, secured a National Science Foundation (NSF) grant for a federally funded research project on how to best implement AI in telehealth by observing doctor/patient communication during telehealth encounters.
Roger Azevedo, the project’s principal investigator and a professor in UCF’s School of Modeling Simulation and Training, described the aim of the research:
“As technology advances in healthcare, it can facilitate ease of use, reduced travel time and more. But there’s also new problems that arise, including the potential for medical errors. We want to use AI to enhance the patient experience, so they get the care they need, and improve the doctor’s experience by facilitating diagnostic reasoning.”
The project’s co-principal investigators were Varadraj Gurupur, an associate professor in UCF’s School of Global Health Management and Informatics; Mark Neider, a professor in and the associate chair of UCF’s Department of Psychology; Mindy Shoss, an associate professor in UCF’s Department of Psychology; and Dario Torre, a professor of medicine and director of Programs Assessment in UCF’s College of Medicine.
Azevedo and team designed a study that would leverage a Telehealth-Neural Network (THNN) model comprised of Natural Language Processing (NLP) and AI-enabled systems to determine the true sentiments of patients and providers and measure data completeness during telehealth encounters.
Communication effectiveness in chat-first care
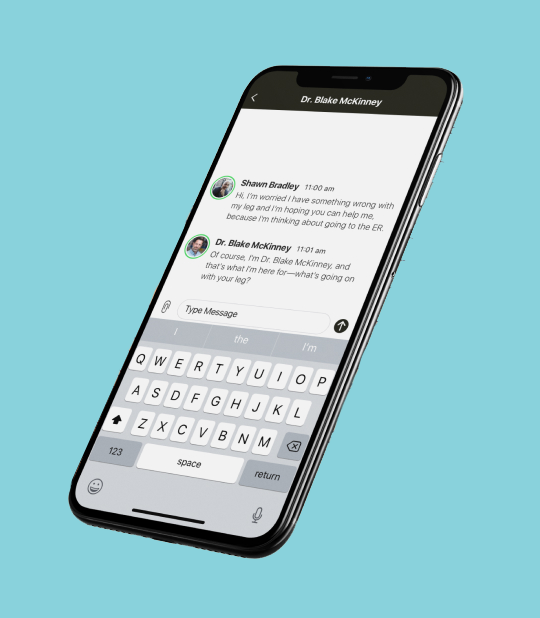
Through CirrusMD’s chat-first platform, a patient connects with a physician in 60 seconds or less and the chat between the physician and patient is stored verbatim in their natural language. If either party failed to document any detail of their encounter, they can refer to the chat text to review what was discussed.
Patient and physician can reconnect during a 7-day window to address additional care needs or concerns that may arise. If a patient has a follow up question, forgot to mention something during the original encounter, or their condition has changed and they need additional support, the physician is only a chat away. The physician can also follow up with the patient to check on progress, treatment results, and adjust as needed.
Supporting the physician is CirrusMD AI which continuously surveys the chat recommending resources and information to the physician that are relevant to the patient’s needs. This takes place in real-time during the care encounter and all recommendations are fully captured, so the patient can easily refer back to them, helping increase the likelihood that referrals are acted upon.
To close the loop, CirrusMD can assign a health coach to help the patient follow through with their treatment plan.

THNN mapping of chat based encounters
THNN mapping of chat based encounters CirrusMD has captured 50M+ one-on-one chat-based exchanges between physicians and patients. Because care episodes are text based and document the exact words communicated, these records are a 100% complete and accurate representation of the encounters.
Upon learning about the research project, CirrusMD reached out to UCF, expressed interest in participating, and the two teams developed a plan for collaboration.
In April and May of 2022, the CirrusMD data team supplied UCF researchers a deidentified data set from the company’s physician/patient one-on-one chat text exchanges, including 84 unique conversations, with a total of 6,259 sentences or lines.
Using the THNN model, Azevedo and team analyzed the CirrusMD chat data set for incompleteness, defined as lost or missing data (for example, a relevant symptom, allergy, or prescription not being documented), and the sentiments of the patients and providers engaged in the chat encounters (the emotions or feelings behind written words).

The findings Azevedo and his team of researchers found
The findings Azevedo and his team of researchers found CirrusMD one-on-one chat text exchanges to have excellent data completeness. This finding indicates clear communication between physicians and patients during the chat exchanges and demonstrates how physicians are thorough in their treatment of patients, as well as their documentation, in the CirrusMD chat modality.
A key resulting hypothesis from this work is that high data completeness correlates positively with patient experience and outcomes because patients receive better care when their history and symptoms are captured accurately.
Azevedo and his team presented their findings at the 44th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC’23), July 24 – 28, 2023, Sydney, Australia, and the study was published in the conference proceedings.
As a result of this collaborative work, the two participating CirrusMD data team members (Christopher Leone, Manager, Data and Analytics; Daniel Schupp, Platform ML Engineer) have been invited to join an IEEE standards working group on electronic health record (EHR) data quality. IEEE is the world’s largest technical professional organization dedicated to advancing technology for the benefit of humanity, with 427,000 members in more than 190 countries.
Additional findings
While not part of the formal study, the patients from the chat dataset provided to the UCF researchers gave CirrusMD a 100% positive patient satisfaction rating and went on to rate the company’s physicians 5 out of 5 in scoring.
Furthermore, the inclusion of text-first colloquial speech, such as emojis, correlates with positive patient feedback CirrusMD has received around physician emoji use. Patients have told the company that the use of emojis makes the conversation feel more human, trustworthy and natural.
“Between the positive sentiment behind our patients’ communication and how they rate their experience, we know our patients have a very positive experience,” said Chris Leone, Manager, Data and Analytics, CirrusMD. “Beyond their positive experience, our patients are also receiving a higher quality of care when you factor in our high data completeness.”
KEY FINDINGS
CirrusMD chat exchanges feature:
• Excellent data completeness
• Thorough physician documentation
• Clear communication between
physician/patient
• Positive patient sentiment
ADDITIONAL FINDINGS
Patients in the data set:
• Gave CirrusMD a 100% positive
satisfaction rating
• Rated CirrusMD doctors 5 out of 5
• Feel physician emoji use makes
chat encounters feel more human,
trustworthy and natural

Industry leading compliance and security
CirrusMD adheres to a robust privacy program in line with the HIPAA Privacy and Security Rules and other relevant state privacy laws. This involves implementing physical, administrative, and technical safeguards within the CirrusMD Provider Network to ensure compliance. The company’s care delivery solution is HIPAA compliant, backed by rigorous HIPAA policies and procedures for effective management and adherence.
CirrusMD maintains its security and privacy programs in alignment with industry standards, evidenced by certifications such as ISO27001 and SOC2 Type II. These certifications attest to the thoroughness in the design and implementation of the company’s policies and safeguards, ensuring they meet or surpass industry norms and are adaptable to evolving threats. To maintain this high standard, CirrusMD conducts annual evaluations and assessments.

Conclusion
The critical role of effective communication between physicians and patients in healthcare cannot be overstated. The research conducted by UCF and CirrusMD provides a valuable exploration of data completeness in the context of virtual care models and sheds light on the pervasive issue of incomplete medical records, emphasizing the profound impact on patient care.
Furthermore, the study’s investigation into the correlation between high data completeness and positive patient experiences and outcomes offers a compelling avenue for improving healthcare delivery.
CirrusMD is now leveraging its smart technology platform and applying AI and ML to its tremendous volume of complete and accurate data to surface valuable insights for doctors to consider in real-time during patient encounters.




